Our study provides an insight into a nationally representative mother–child dyad sample of India in terms of their coverage by a sequence of maternal, newborn and child health (MNCH) care services, also commonly referred to as Continuum of Care (CoC). Nineteen sequential MNCH services were considered in the CoC. Only a minority of mother–child dyads received all the 19 interventions, half of the dyads received 14 out of 19 services and 10% dyads received only 9 interventions.
Among the most frequently accessed services were sterile delivery kit usage, recording weight of newborns and skilled birth attendance—all three interventions related to the intra-partum phase. The greater coverage by delivery-related intra-partum interventions were reported by others also [10, 23, 24]. The highest coverage by the intra-partum interventions perhaps can be attributed to various financial incentives provided to pregnant women conditional on their utilization of public institutional delivery services, such as Janani Suraksha Yojana [39, 40] and Pradhan Mantri Matru Vandana Yojana [41].
Early initiation of breastfeeding, minimum four ANC visits, appropriate iron-folate consumption and information about pregnancy complications were the least frequently accessed interventions. Existing socio-cultural norms and misconceptions have strong unfavourable influence on breastfeeding-related behaviours (such as “early milk or colostrum is not good for newborn”) [42, 43] and iron-folate consumption (“iron turns stool black”) in many LMICs including India [44]. These can be only overcome by quality counselling, which can be administered during multiple contacts between the would-be mother and healthcare workers during ANC sessions. The low coverage of four stipulated ANC sessions and subsequent lower coverage of counselling points (such as danger signs of pregnancy) that we observe in our study, perhaps “triggers” disruption in subsequent interventions, explaining low early breastfeeding and iron-folate consumption rates among Indian dyads. Similar correlation between counselling and downstream ANC, PNC components were reported by others [45, 46].
At national level one fourth of the variation in the CoC score was explained by the state effect. This shows that despite wide variations of poverty, education, caste and urbanization of their citizens across the Indian states, the state health system—state effect being a surrogate measure of the strength of state health system—can shape CoC coverage. So, by further strengthening outreach facilities of the health system (the place dimension of CoC) and ensuring timely provisioning of the chain of interventions (the time dimension of CoC), the welfare state can impact MNCH coverage of the mother–child dyad substantially and equitably. Almost no attenuation of the “state effect” (from only 27% to 25%) after adjustment with socio-economic variables further confirms that the effect of the state health system is largely independent of the socio-economic situation of their residents.
Odisha which is one of the eight Empowered Action Group (EAG) states—the Indian states with less socio-economic development and therefore higher priority—illustrated the best state effect. More prosperous southern and western Indian states are anyway expected to experience better coverage because they are home to richer, more educated and urbanized people. This was visible in the crude ranking that was dominated by these richer states. But even in that list Odisha ranked seventh (mentioned in the legend of Fig. 4). And after adjusting for differences of structural determinants, performance of EAG states like Odisha, and also to some extent Chhattisgarh and Madhya Pradesh are encouraging, which is a novel insight from this study. It shows, despite smaller fiscal space, poorer states can also achieve significant public good. But also, at the same time, other large EAG states like Bihar, Uttar Pradesh, Rajasthan and Jharkhand and almost all North–Eastern states (except Sikkim) could not achieve what Odisha could and continue to languish in the sub-national zone of achievement.
The public private conundrum
In this connection it is important to note that in addition to the public healthcare sector, broadly speaking, the health system in India comprises a significant private sector which varies widely across states in terms of its size, level, reach, system of medicine, quality and the regulatory framework it operates within [47]. So, the moot questions are, is the good performance of the poorer EAG states like Odisha and few others mainly due to the strength of their public sector and what is the role of the private sector in their achievement?
We conducted some post-hoc analysis to answer these questions. The NFHS-5 data has public/private information for ANC services, place of delivery and immunization. Observation of public/private usage (Supplementary Table 2) showed that there is no clear correlation between private contribution and the economic status of the state. Private is naturally higher in richer states like Kerala (ANC private: 50.3%, Delivery private: 61.4%, Vaccination private: 11.8%), Goa (28.6%, 37.5%, 6.4%) and Gujarat (40%, 51.4%, 6.6%), because in India private healthcare sector is perceived to be of better quality although expensive and therefore more people from these affluent states prefer to seek care from private sector, despite strong presence of public sector in these states. But also, we observed high private sector usage in poorer EAG states like Bihar (36.2%, 18.9%, 2.8%) and UP (26.5%, 25.8%, 5%), which may be due to weakness of public sector in those states [48]. But most importantly, we observed high public sector usage in the better performing EAG states like Odisha and therefore low contribution by private sector (15.8%, 12.7%, 1.2%) Chhattisgarh (10%,13.6%, 2.7%) and Madhya Pradesh (17.7%, 10.7%, 1%). Additionally, we adjusted for the public/private contribution to these three services in our second model that was used to estimate the state effect and the adjusted rank of the states. The state effect hardly changed after adjustment with public/private variables, nor did the ranks of the states (Supplementary Table 2). Therefore, most likely the achievement of good performing EAG states like Odisha and few others, which had high public sector usage, were achieved by investing in and strengthening their public health system. Whereas the poorer EAG states like Bihar and UP perhaps underperformed because of weaknesses of their public sector, although more research in future is needed to disentangle this public/private contribution to CoC coverage.
Policy implications and future actions
Our results have the following policy implications. First, coverage of all mother–child dyads by all the MNCH interventions is yet “some way to go” in India, especially counselling-based services. Counselling is a higher-level skill [49] but the dependence of the Indian rural public health system on less-skilled frontline workers like Accredited Social Health Activist (ASHA) poses a challenge to the quality of counselling. How the ASHAs can be equipped with adequate counselling skills should be an important policy agenda, especially in less-developed states, because quality of counselling can “make or break” many health programmes.
Second, under-performing less-developed states like Bihar, Uttar Pradesh, Jharkhand and Rajasthan and almost all the North-Eastern states can increase their CoC coverage rates by strengthening their health system. This can be achieved even with limited fiscal space as Odisha has demonstrated, however, special federal assistances for poorer states may be considered as and when necessary. Such health system enhancements in less-developed states can perhaps address in future the tenacious regional inequities that exists across the nation and nudge India towards equitable and universal coverage of MNCH services.
Our methodology for eliciting adjusted state effect—or contextualized value addition by the state as the education literature would call it [36] can be adopted by policy makers, especially while ranking states for various purposes. For example, the National Institute for Transformation of India (NITI), the apex governmental policy thinktank, ranks Indian states based on various health-related indicators (not only MNCH), where this methodology based on multi-level models can be applied.
Future research should focus on explaining why some less-developed states could achieve high CoC coverage whereas others could not. One should study what health system levers were activated to achieve success in those high achievers. To what extent this coverage is getting transformed into maternity and child health outcomes is another critical yet unanswered question, which future research should also address.
Limitations and strengths
However, our study has few limitations, first, it could not estimate the coverage of a critical indicator, exclusive breastfeeding, because of the design of the study. The exclusive breastfeeding question was only asked to children of the age of 0–6 months (“what food other than breastmilk was given to the child in the last 24 h?”), but since our sample included children 12–23 months old at the day of interview, they were not administered that question, hence we could not measure exclusive breastfeeding. Another limitation of our analysis, we could not explore to what extent the state-wise variation in out-of-pocket expenditure related to MNCH services tracked the CoC score. The OOPE data was available only for delivery-related (intra-partum) services and not for other components of CoC. Future studies may take the OOPE issue into account.
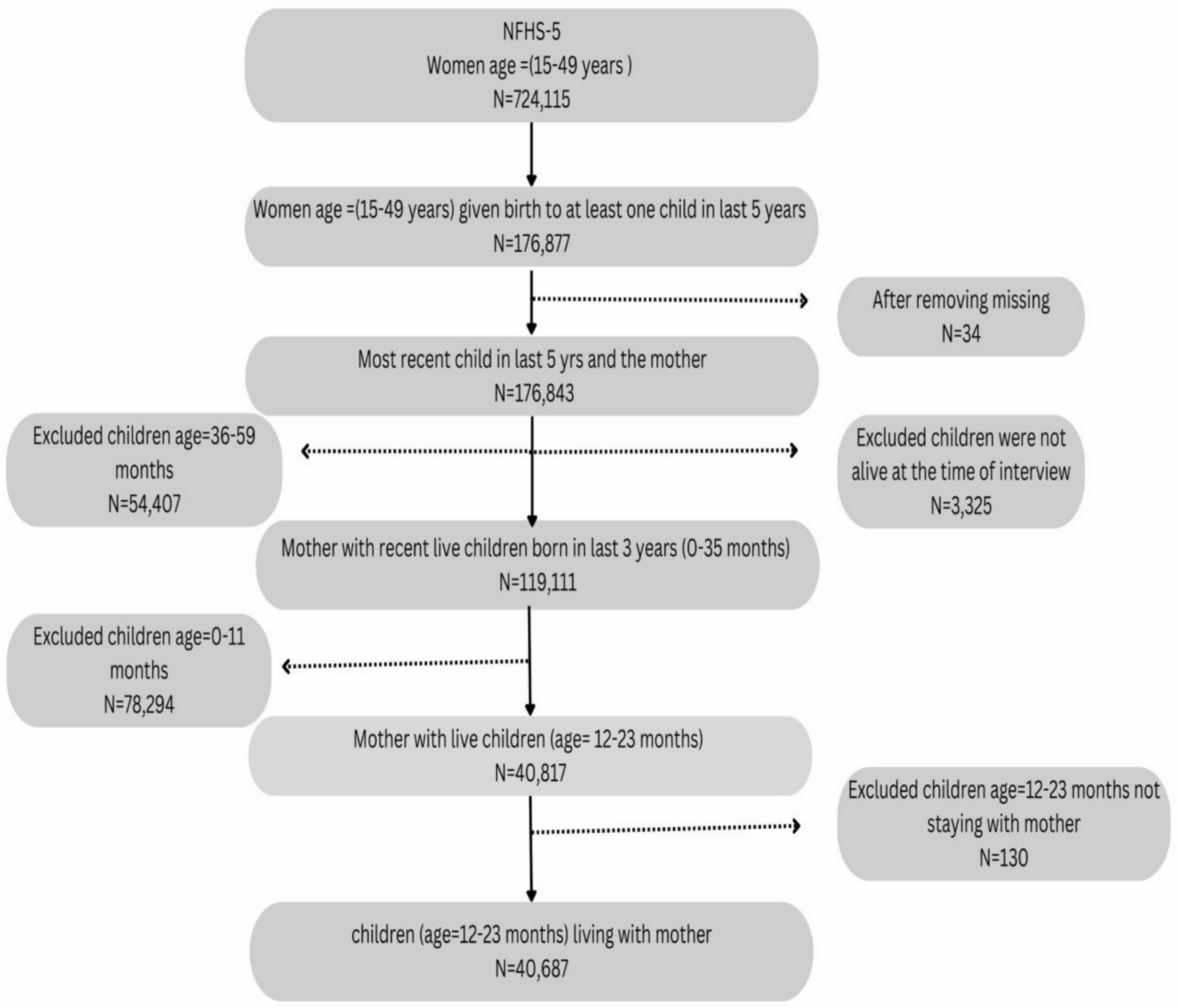
Our study has the following strengths. First, the socio-economic and other attributes of our sample of mother–child dyads (n = 40,687) were similar to all the NFHS-5 mothers (n = 176,843) who had given birth to live children in the last five years (Table 1). This has demonstrated that the dyad-level coverage scores we have reported in this article and then used as an outcome for further analysis, were not affected by any selection bias. Second, all the CoC indicators used in our study are globally harmonised standardized indicators from the family of Demographic and Health Survey affording cross-country comparison and within-country comparison of geographical units. But most importantly, our composite score, which is an unweighted cumulative count of 19 interventions estimated at the individual-level (mother–child dyad level), has a few advantages over the frequently used aggregate-level composite scores like CCI. Only individual-level scores like ours can be used to generate the following evidence “In the 2013 Nigeria DHS, 13% of mothers and children failed to receive any of the interventions, of whom 64% belonged to families in the poorest quintile.” This was pointed out by Wehrmeister et al. when they used the above statement as an example to illustrate the strength of individual-level composite score-based analysis as a tool for advocacy from the rights perspective. Aggregate-level scores like CCI cannot be used for such critical inferences. Also, like CCI, individual-level score can be used to review the performance of higher-level units like countries, states and districts, but additionally the comparison using individual-level score can be adjusted for differences across units, like we have done in this manuscript, which could not have been done with CCI. Lastly estimation of standard errors of aggregate-level CCI is complicated, whereas computing standard errors for individual-level composite score is much more straightforward. One can argue that a score of 10 out of 19 of a dyad does not reveal in which stage of CoC the deficiency lies for that mother–child pair, but that is a weakness of any composite core, be it individual or aggregate-level. For that purpose, coverage of each intervention has to be assessed, which is anyway routinely done in MNCH programmes. Composite scores are primarily for spatial comparisons, comparison between groups from equity angle and/or tracking trends towards certain global goals such as SDG; and additionally individual-level scores can generate powerful rights-based insights as explained above and can be used for ranking geographical units based on their adjusted performances.