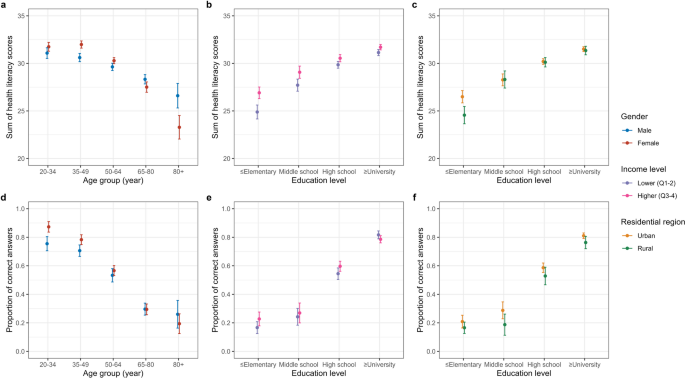
The results of our study revealed that older age (≥ 65 years) was negatively associated with health literacy scores. Female gender was positively associated with overall health literacy among younger individuals but showed a negative association in older age groups. Both higher income and higher education levels were positively associated with health literacy. The model based on the total health literacy score included age, gender, income, and education, along with interaction terms for age and gender, and for income and education. The model based on the knowledge assessment included the same four sociodemographic variables and, additionally, residential region, which was found to be a significant factor. Interaction terms were not included in the final model for the knowledge-based assessment.
Consistent with previous research, older age, lower education level, and lower income level were associated with lower health literacy scores. Interestingly, the effect of gender was positive for younger age groups but reversed in older age. In addition, the effect of region was not significant when education level and income were considered. It is noteworthy that the Technology and Resources domain was more affected by other domains of health literacy, and this trend was further emphasized in the knowledge assessment.
Lower health literacy in the elderly has been an ongoing concern. A previous study highlighted that inadequate health literacy in the elderly is an independent predictor of all-cause mortality and cardiovascular death22. It is alarming that this issue is even more pronounced with digital technologies, and measures to improve digital health literacy are required23,24. The lower health literacy in elderly females may be associated with lower proficiency in mobile device use among females25and it is expected that this trend will decrease in younger age groups.
There has been ongoing debate regarding gender differences in health literacy. A systematic review focusing on individuals with migrational backgrounds suggested that men may have lower health literacy compared to women26. In contrast, another study of hospitalized older patients with chronic diseases found slightly higher health literacy levels in men, though the difference was not statistically significant26. Recent studies on gender differences in health literacy, including digital health literacy, have reported highly variable findings27,28. These inconsistencies suggest that the effect of gender on health literacy may depend on other sociodemographic factors such as age, cultural context, and the specific measures of health literacy used. Our study supports this notion by demonstrating a significant interaction between age and gender in the total health literacy score (Table 2), whereas the interaction effect was not significant in the knowledge assessment model (Table 3; Fig. 2).
The digital divide related to education level is highly concerning. In our analysis, the effect of higher education level was the strongest in both health literacy measures. This trend was most evident in the Technology and Resources domain and in the knowledge assessment based on digital tools. A similar trend has been observed in other countries29,30. It is alarming that this divide could bias the data collection process in clinical trials where digital health technologies are widely and increasingly used31. Therefore, equitable access and the inclusion of diverse trial participants should be carefully considered when implementing digital health technologies32.
The effect of residential region is also noteworthy. As shown in Table 2, rural residential region was not significantly associated with health literacy measured by self-reported questionnaires. However, it was significantly negatively associated with health literacy in the objective knowledge assessment. Therefore, the characteristics of each health literacy measure should be carefully considered when interpreting the results33. Additionally, the results suggest that “sufficient” health literacy reported by participants does not always reflect proper understanding, as similarly observed in a trial using electronic consents18.
We also found that the effects of sociodemographic determinants varied depending on the measure of health literacy used. Notably, the odds ratios for older age (Fig. 2) showed contrasting directions between the health literacy measure Q1 (“Can you assess which vaccinations are necessary?”) and other measures, suggesting a measure-dependent nature of health literacy. Additionally, the magnitude of these effects varied across different measures, with the knowledge assessment showing the largest effect size for older age. Therefore, health literacy results should be interpreted cautiously, considering both individual items and overall trends. This perspective aligns with a systematic review that highlighted the inconsistent correlation between self-reported and performance-based health literacy measures in relation to health outcomes15.
Our study has several limitations. First, the health literacy instrument used (HLIC) was introduced relatively recently. Although it has been validated in a small sample with characteristics similar to those of the KNHANES population, further validation studies are needed. Additionally, as this was the first use of the instrument in the national survey, temporal assessments were not available, which limits the ability to assess the stability of the results over time. Intercultural and interethnic comparisons are also necessary to determine the generalizability of the findings to other populations.
Second, although KNHANES includes a large, nationally representative sample of the general Korean population, it may differ from clinical or patient populations to which the results may be more directly applicable. While the representativeness of the sample could potentially be supported through linkage with nationwide claims data, health literacy was not assessed in patient-based datasets. Finally, the retrospective design of the study limits the ability to establish causal relationships. Further prospective studies in patient populations are warranted to explore the relationship between health literacy and health outcomes more thoroughly.
In conclusion, we demonstrated that older age, lower education level, and lower income level are associated with lower health literacy. The effect of gender on health literacy varies across age groups. The association between age and education level is particularly strong in digital health literacy.