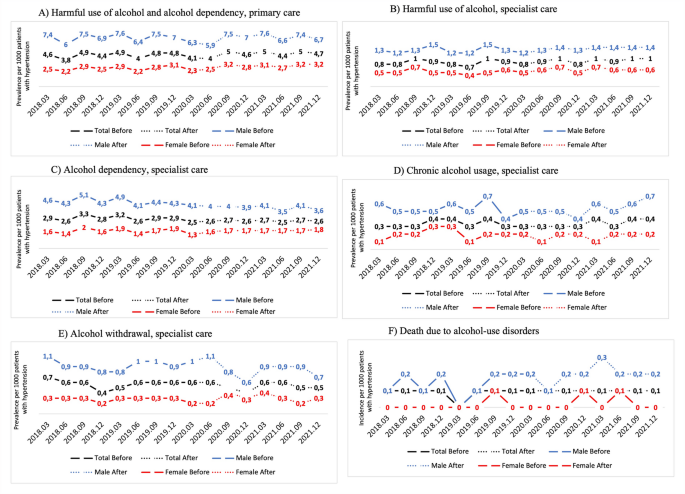
From a public health perspective, and considering potential prevention strategies, this study focused on a vulnerable group—patients with hypertension. Our main finding revealed no profound shift overall in alcohol-related disorders or deaths from the causes studied during the pandemic compared to the pre-pandemic period. However, some changes were apparent. In female participants, the quarterly period prevalence of alcohol-related disorders in primary care showed an upward trend. In contrast, the trend of alcohol dependency in specialist care appeared to decline, particularly in males. Both during the pandemic and the pre-pandemic period, the general rates of all alcohol-related disorders and alcohol-related deaths were higher in males than in females. In addition, among other alcohol-associated conditions, cardiovascular disease exhibited an increasing trend in both sexes in primary care and in males in specialist care. Mental illness showed decreasing trends in both sexes, particularly in specialist care.
To our knowledge, this is the first study to examine pandemic-related trends in alcohol-related disorders among participants with hypertension, a large and heterogeneous group particularly vulnerable to alcohol. Unlike a study conducted in the general U.S. population, which covered a similar pandemic period as ours 31, we did not find any increase, but rather a decrease in males, of any of the alcohol-related disorders in specialist care. The US study, which employed a longitudinal interrupted time series analysis, reported significantly higher-than-expected rates of alcohol-related complications during the pandemic for both males and females, with significant increases particularly among females aged 40 to 64 31. In alignment with these results, a meta-analysis on alcohol intake showed an increase of harmful drinking in the US, but no increase has been reported in Europe 20,32,33.
In our study, we observed an upward trend in alcohol-related disorder diagnoses in primary care among females. This increase may not be directly related to the pandemic, but rather reflects a broader pattern in Sweden. Between 2011 and 2022, 15.6% of the Swedish general population reported hazardous alcohol use. While the prevalence has declined in men, it has remained unchanged in women 34. Additionally, hazardous alcohol use is more frequent in individuals with hypertension compared to the general population 7. In Sweden, approximately 27% of adults have hypertension 35, with most cases managed in primary care 36. Primary care plays a vital role in addressing lifestyle factors and promoting healthier habits, such as reducing alcohol consumption 37; however, this was disrupted during the pandemic and could contribute to shifts in alcohol-related disorders.
We found that death due to alcohol-related disorders did not change during the pandemic in either sex. This finding aligns with data from two other Scandinavian countries, Denmark and Finland, included in a meta-analysis 38. In contrast, alcohol-attributed deaths increased in the US 39 and some European countries, particularly the Baltic countries, Bulgaria, and Spain 38. It is important to consider that some alcohol-related disorders may have been categorized as COVID-19 cases on the death certificate during the pandemic when these conditions co-occurred.
Our study found that most other alcohol-associated conditions decreased across healthcare settings during the first six months of the pandemic. However, as the pandemic progressed, the periodic prevalence of many diagnoses returned to pre-pandemic levels, with one notable exception: cardiovascular diagnoses, which increased in both sexes in primary care and in males in specialist care. This trend was observed across all healthcare settings and may be attributed to delayed care during the pandemic 24,40, as healthcare systems focused on controlling COVID-19, reducing routine screenings and diagnostics 41. In Sweden, the overall rate of physical healthcare visits decreased during the early phase of the pandemic, as the Public Health Agency recommended in March 2020 that all non-essential care should be postponed 42. This likely affected the management of patients with alcohol-related disorders and chronic cardiovascular diseases, and may also have delayed the diagnosis of new cases.
Once healthcare services resumed normal operations, these common diagnoses increased as patients finally sought care 43, potentially leading to missed opportunities for preventive cardiovascular care in individuals with high risk. The long-term health consequences of decreased prevention during the pandemic remain unknown.
In line with another Swedish study in the general population 44, we observed that hospitalization rates for cerebrovascular disease remained stable among subjects with hypertension during the pandemic, comparable to the pre-pandemic period. In terms of mortality from cardio- and cerebrovascular diseases, our study found no significant change in deaths during the pandemic compared to the pre-outbreak period. These findings align with results from the Swedish national registry study in the general population, which reported no significant change in death rates due to cerebrovascular and cardiovascular diseases, with a slight trend towards a decrease 45.
Our study found that the periodic prevalence of the most common mental illnesses, depression and anxiety, decreased in both males and females with hypertension early in the pandemic and stayed lower than before by the end of the pandemic study period, especially in specialist care. Patients with emerging mental health or substance-related conditions may have postponed seeking care, resulting in delayed identification of these diagnoses. We showed that, similar to pre-pandemic trends, the occurrence of diagnoses of depression and anxiety continued to be higher in females than in males. The association between alcohol-related disorders and depression and anxiety is well-documented 46. Although fears, financial concerns, and isolation during the pandemic were thought to harm mental health 47, a survey study across six countries, including Sweden, found no overall change in depression and anxiety symptom rates, apart from higher symptom rates in those with self-reported prior diagnoses of depression/anxiety 48. Similarly, a United Kingdom (UK) study reported fewer newly diagnosed psychiatric diagnoses during COVID-19 49. As an explanation, it has been suggested that individuals with milder mental health issues may have sought alternative coping mechanisms outside of medical intervention. Additionally, access to healthcare was limited due to the prioritization of COVID-19 24,40.
Our study also showed that female participants were more frequently diagnosed with COVID-19 in primary care throughout the pandemic, while male participants were more commonly hospitalized due to the infection. This finding aligns with previous meta-analyses indicating that males accounted for a higher proportion of severe and critical cases 50. Mortality rates in our study varied between hypertensive females and males, depending on the study period. This pattern contrast with the general population, where both international and Swedish statistics reported that male mortality rates were up to twice as high as those for females during the pandemic 51 This difference might be explained by the fact that hypertensive patients often have additional chronic conditions compared to the general population 52, a pattern also observed in our study cohort.
We further demonstrated that the cumulative incidence of injuries and accidents requiring emergency care or hospitalization increased in the latter part of the pandemic for both sexes, compared to the pre-pandemic period. Previous research suggested that as people spent more time at home, there was an increase in domestic injuries and accidents, especially falls and ingestions, while vehicle-related accidents declined 53,54. Despite this increase in non-fatal incidents, we observed that deaths due to injury and accidents remained unchanged during the pandemic compared to pre-pandemic levels. In Sweden, strict lockdowns were not implemented, and mobility restrictions were less pronounced than in many other countries. Our findings highlight the complex and context-specific impact of the pandemic on accident and injury epidemiology, and underline the importance of considering national strategies and healthcare-seeking behaviors when interpreting the results.
Hazardous alcohol use has also been strongly linked to suicides—evidenced by a pre-pandemic meta-analysis showing a 94% increase in the risk of suicide related to alcohol use 13. The COVID-19 pandemic represented a unique societal event that may have influenced these outcomes in complex ways. Therefore, given the established association between alcohol use and an elevated risk of suicide, we also analyzed suicide-related deaths. Our findings revealed that, as in the pre-pandemic period, suicide rates fluctuated and remained consistently higher in males than in females. Despite concerns that social isolation and economic stress would increase suicide rates, both our findings and others in the general population indicate that suicide incidence remained stable during the pandemic 55. This suggests that while alcohol use is a well-established risk factor for suicide, the pandemic did not substantially alter overall trends in suicide mortality, at least in the short term.
The clinical relevance of our findings lies in their ability to inform tailored prevention and management strategies for hypertensive patients, a population already at heightened risk for adverse cardiovascular outcomes 5. The observed sex-specific differences—such as the rise in alcohol-related disorders in females within primary care and the increase in cardiovascular diagnoses among males in specialist care—highlight the need for gender-sensitive approaches in clinical practice. These insights reinforce the critical role of primary care in addressing lifestyle factors, such as alcohol consumption, which remains a modifiable risk factor for cardiovascular disease 7. Elevated blood pressure remains the leading preventable cause of cardiovascular mortality globally 2. Moreover, the study underscores the broader impact of the COVID-19 pandemic on healthcare delivery, emphasizing how disruptions in routine care may have contributed to delayed diagnoses and potential missed opportunities for preventive interventions 24,40. Long-term cardiovascular monitoring of hypertensive patients is essential, as the pandemic may have compounded risks through increased stress and lifestyle changes such as reduced physical activity and altered nutrition.
Furthermore, COVID-19 itself may result in long-term health effects, including hypertension, other cardiovascular disorders 56 and post-COVID-19 condition 57. These findings stress the importance of maintaining uninterrupted care for chronic conditions during public health crises and highlight the need for further research to fully understand the long-term health consequences in vulnerable populations. Further research—including studies covering the post-pandemic period and incorporating risk factors other than alcohol—is necessary to fully understand the impact of the COVID-19 pandemic and its countermeasures on other alcohol-associated conditions, including cardiovascular diseases, in the population.
The strengths of our study lie in the use of comprehensive, large population-based data on patients with hypertension from both urban and rural areas within Region Stockholm, Sweden. This approach ensures robust representation across different age groups and sexes, enabling a detailed examination of trends over time in females and males. The repeated quarterly data from the Swedish national registers also allow for unique insights into the various phases of the pandemic. Our analysis also captures diagnoses originating from both primary and specialist care settings.
This study has several limitations, primarily due to its descriptive and exploratory character, which restricts causal interpretations of the observed trends. Another limitation is that our data did not capture alcohol-related disorders for patients who did not seek medical care. While surveys can provide such information, our findings align well with survey-based study findings. Furthermore, we did not account for different virus variants across the quarterly periods. We did not account for possible changes in attainment of blood pressure targets, a phenomenon observed in the Stockholm Region during the pandemic 58. We did not adjust for antihypertensive treatment as a variable in our analyses. Although treatment status could be represented as a binary factor, accounting for it properly would require a different study design to disentangle treatment effects from underlying disease severity and health-related behaviors, which is a different scientific question. Finally, our register-based study did not account for other lifestyle factors that may have changed during the pandemic, such as decreased physical activity, altered nutritional behaviors, or an increase in BMI, which could all contribute to different health trajectories in hypertensive individuals.