The contribution of amblyopia visual impairment is not usually considered in meta-analysis data, especially since most of its contribution is unilateral visual impairment. In TMES, amblyopia visual impairment was a unilateral condition in 97.8% of times and its contribution to unilateral visual impairment (when defined as > 0.5 logMAR) at 38.8% (95%CI 30.5%-47.6%) seems higher to that of similar studies in populations aged 40+, using > 0.5 logMAR best corrected visual acuity threshold, reporting 18.9% (95%CI 10.7%-29.7%)28 and 15.8% (95%CI 7.5%-27.9%)29. When compared to The Casteldaccia Eye Study, which also used the ICD-11 criteria for visual impairment severity, the amblyopia contribution to unilateral moderate severe visual impairment was similar in both studies (TMES: 34.8%; 95%CI 25.0%-45.7%; Casteldaccia: 29.5%; 95%CI 16.8%-45.2%), but its contribution towards unilateral blindness was higher in TMES (TMES: 45.7%; 95% CI 30.9%-6.0%; Casteldaccia: 3.3%; 95%CI 0.1%-17.25)28. Amblyopia as a cause of unilateral blindness (> 1.0 logMAR) was also lower in studies such as the Blue Mountains Eye Study (13.3%; 95% CI 7.8%-20.7%)30. The higher rates observed in TMES may potentially relate to historically lower availability of vision screening and amblyopia treatment in Malta compared to countries such as Australia, as well as a possible higher prevalence of anisometropia in the same age group in Malta (22.1%) than in Australia (14.1%)31. Moreover, unassessed parental factors, such as socioeconomic and educational status, smoking, diet, genetic factors and foetal development in utero could possibly account for such differences in amblyopia rates. Conversely, the similarity with the Casteldaccia Eye Study may reflect comparable healthcare contexts and methodologies.
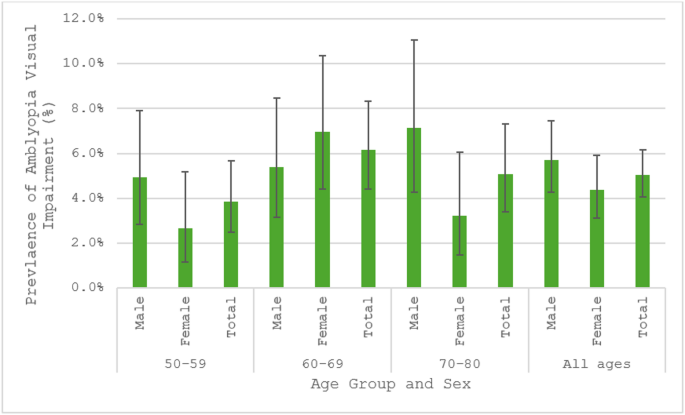
The 60–69-year age group had double the odds of amblyopia visual impairment vs. no visual impairment compared to the 50–59-year age group. This finding likely reflects differences in childhood eye care provision across age groups, although causality cannot be established. Amblyopia treatment is most effective before the age of 732,33,34, and individuals aged 60 years and older during TMES’s data collection period (2021–2024) would generally have passed this critical window before structured paediatric eye care was widely available in Malta.
In the early 1970s, national orthoptic services were introduced and, at the time, refraction in children was performed primarily by orthoptists, with only a small number of ophthalmologists and optometrists providing this service. While strabismus was not the major cause of amblyopia in this population, the shared role of orthoptists in detecting and correcting refractive errors, including anisometropia, suggests that these services may have contributed to a reduction in amblyopia-related visual impairment in younger age groups. However, it is important to note that other explanations are equally plausible, including broader improvements in health literacy, healthcare access, increased accuracy of refractive assessment, and greater availability of corrective lenses.
Similar age-related differences in amblyopia prevalence across age groups have been observed in other populations35, highlighting the complexity of separating the effects of specific healthcare services from broader improvements in paediatric eye care. The decline noted in the 70–79-year group may additionally reflect diagnostic challenges in older adults, survivorship bias, or opportunistic screening during trachoma eradication efforts in the 1940s and 1950s36–38. These multiple factors highlight the difficulty of attributing age groups differences to any single intervention.
Since there are no management options for amblyopia visual impairment in adulthood, and amblyopia in adulthood reflects previous childhood eye care, TMES’s amblyopia findings can suggest further investigation of amblyopia prevalence in childhood in Malta. Apart from the orthoptic department setup in the early 1970s, Malta has also seen the introduction of childhood screening39 and paediatric ophthalmology services over the past 30 years. As a result, lower amblyopia prevalence rates are expected in both the current younger population and the future older generations. The absence of prevalence data in current younger age groups in Malta limits direct comparison, and further research on current amblyopia and visual impairment rates in children and young adults would help quantify the impact of improved paediatric eye care services.
The causes of amblyopia in the TMES population were similar to those reported in other populations30,40], with anisometropia as the predominant factor. However, its true prevalence may be underestimated because of limitations in accurately identifying past paediatric anisometropia in this older population.
Although individuals with amblyopia-related visual impairment reported statistically significant reductions in several NEI VFQ domains, the magnitude of these differences was very small (all r² values < 0.01) and below the threshold generally considered clinically meaningful (≈ 3 points on the NEI VFQ scale)41. This suggests that while subtle quality-of-life differences may be detectable in large samples, amblyopia has only a limited impact on vision-related quality of life in adulthood. These findings should be interpreted cautiously given the exploratory nature of multiple comparisons and the minimal variance explained by the observed effects. A smaller Munich study found no differences42, our larger sample size likely enabled detection of these small effects, though their clinical importance remains limited.
Strengths and limitations
The strengths of this study include its large, population-based design, evaluation of functional outcomes such as vision-related quality of life, and its focus on amblyopia in older adults, a group often underrepresented in research. The study was also clinician-led, with all examinations conducted by the same specialist, minimising inter- and intra-observer variability16, and enhancing the robustness of the findings.
In some cases, coexisting ocular conditions (e.g., cataracts) may have contributed to visual loss, confounding the role of amblyopia. To minimise misclassification, a stricter threshold of > 0.3 logMAR was used, rather than the > 0.2 logMAR typically applied in paediatric settings3,43], to enhance specificity in adults.
Classifying amblyopia causes in older adults is challenging because age-related ocular changes obscure the original aetiology. Cataract surgery and lens changes can mask or induce anisometropia, whereas lifetime refractive shifts further complicate the identification of anisometropic amblyopia. Strabismus classification is limited by changes in alignment, surgical history, and natural evolution over time. Strabismus assessment relied on the Hirschberg test, which may have underestimated small-angle deviations. Additionally, degenerative changes in amblyopic eyes, particularly in those with high myopia, can mimic or mask amblyopia-related vision loss. The lack of pre-and postoperative cataract refractive data, availability of binary childhood vision loss history, and absence of detailed squint records limited precise causal attribution. As a result, anisometropic amblyopia may have been underreported, particularly in pseudophakic individuals. Future prospective studies with longitudinal data and comprehensive ocular histories are needed to improve classification accuracy, as the retrospective design limits causal inference owing to potential bias, confounding, and unclear temporal relationships.
A limitation of TMES is the lack of comparative prevalence data in younger age groups, such as those aged 20–30, who have had the benefit of modern paediatric eye care services. Future studies assessing visual impairment and amblyopia prevalence in these younger generations are required to contextualise the improvements achieved in childhood eye health.
This study used participants’ employment status and educational level as proxy measures for socioeconomic circumstances. However, parental socioeconomic status would have been a more accurate indicator for amblyopia, as current status may not reflect childhood healthcare access.