The last time you met with your doctor, they may have asked for permission to have an ambient listening tool tune in to the conversation.
If you said yes, that means an Artificial Intelligence recorded your conversation and then produced a concise, comprehensive report summarizing it. Your physician then reviewed the report before uploading it to your file.
Terry Purcell, Regional COO for Jefferson Health–Lehigh Valley Region, says the tool is saving each of his physicians an average of four hours per day, time which is used to see more patients. It also helps physicians divest their full attention in the patient and their needs during a visit, rather than meticulously taking notes, resulting in greater satisfaction on both ends.
And notetaking is just the beginning of how technological innovation is impacting medicine in Schuylkill County.
For the county’s small, rural and sometimes remote communities, technology in medicine is becoming a connecting force, bringing care that is increasingly more accessible, safe, efficient and of high quality to residents. And in multiple ways, the innovation is helping address the critical needs of a community that has historically lacked extensive regional care.
“Healthcare is changing, and the unique is becoming the normal now,” said Michael Peckman, Director of Communications and Community Engagement at Jefferson Health. “It shows that all of this technology in healthcare is available everywhere in the country, including to a rural Schuylkill County.”
Prior to the visit
Technology is all about getting ahead of the game.
At St. Luke’s Health Network, which has hospitals in Orwigsburg and Coaldale, health centers in Pottsville, Tamaqua and Mahanoy City, and a family practice in Ashland, “multi-channel” engagement tools are impacting patients’ experiences before they even step into a waiting room.
Charles Sonday, Associate Chief Medical Information Officer at St. Luke’s, says digital tools are improving information accessibility through MyChart, the online database where patients can view their test results, appointments, bills and more. According to Sonday, approximately 80% of St. Luke’s patients have a MyChart account, a number that has surged since the COVID-19 pandemic.
For example, AI-powered agents are available to help patients find appointment times that accommodate their schedule, or to notify those on an automated waitlist of new appointment openings in real-time.
Digital tools also exist to help folks navigate the sometimes disorienting financial side of medicine. Insurance coverage for a procedure or visit is confirmed ahead of time through a patient’s electronic medical records, boosting transparency and helping avoid unexpected bills. Later on, if a patient has questions after receiving their medical bill, they can even talk or text with an AI-powered agent to gain clarity on its breakdown.
“It’s more of an upfront process so that you know as the patient that everything is going to be covered,” Sonday said, “providing really more of an interface that allows the patient to ask multiple questions and find out multiple answers before they may even be in the visit.”
Addressing needs
“My mom went to our campus that’s in Schuylkill County, and she needed to see a neurologist,” Sonday shared. “The neurologist saw her the same day that she was admitted, because we were able to do a virtual teleconference visit with that neurologist. Instead of taking two hours to get there because they were on the other side of the network, we were instantly there.”
For networks serving Schuylkill County, stories like this are what innovation in medicine is all about.
Folks in rural areas, like Schuylkill County, are more likely to have to travel further distances to receive medical services, especially if they are seeking specialized care, such as cardiology or neurology services. For older folks, of which there are many in the region, travel can be particularly difficult or even inaccessible.
Data from the National Rural Health Association suggests that for every 100,000 people living in an urban area, there are an average 260 specialists; but for every 100,000 people living in a rural area, there are an average 30 specialists.
However, technology is helping bring more critical caregivers to the area, allowing patients and their families to remain closer to home.
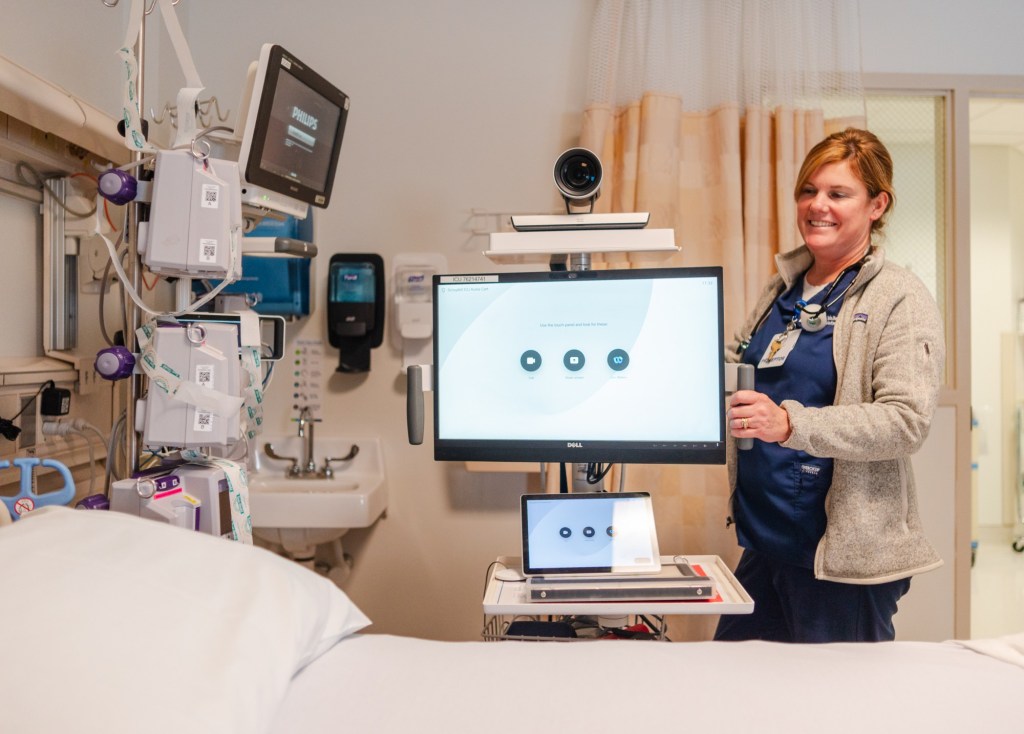
The Hicuity Tele-ICU has been in use at Jefferson Health for a few years now, and is composed of a monitor on a rolling desk that can be moved from room to room in the ICU. Out-of-region intensivists can engage with ICU patients and their bedside providers, say, in Pottsville, through telemedicine calls. The intensivists or a remote care team can monitor the patient’s condition and even initiate medical interventions if abnormalities are detected.
Upgrades to imaging technology that detects cancer also carry particular weight in the region. According to Purcell, Schuylkill County cancer rates are high — the county has the Commonwealth’s second highest cancer rate in men and fifth highest in women.
Jefferson Health’s PET scans, which detect tumors and are often the first line of defense against cancer, have been upgraded network-wide in the last year.
“Having comprehensive cancer services are very important… we’ve been on a mission to upgrade all of our technology in the hospital,” Purcell said. “The new MRI is only a couple years old, new CAT scans (are) coming. We’re very proud that we offer the latest and greatest technology to our patients.”
New possibilities
Not only is technology helping to make healthcare more accessible and efficient, but it is even pushing the boundaries of what is possible in local medicine.
At Jefferson Health, robots are assisting with surgical work. Last fall, the network upgraded all 18 of its robots to the latest model, the da Vinci 5. Though the network has used these robots for around 15 years, the latest technology has 10,000 times the computing power of previous models, magnified 3-D vision and advanced depth perception, ultimately producing stronger results.
With a technology called Force Feedback, the robot exerts 43% less pressure on human tissue, helps reduce surgeons’ natural tremor and can create smaller incisions than typically possible. In turn, patients’ recovery periods are shorter, according to Purcell.
Notably, medical officials emphasize that tools like these are not intended to replace humans — they are applied as an aide, intended to enhance medical services.
An AI tool at St. Luke’s is even proving life saving in some cases. A piece of technology that attaches to a patient’s finger, the tool performs constant monitoring of their vitals and jumps to action when abnormalities pop up, sending an automatic alert to medical staff to intervene before complications grow severe.
According to an article in the Philadelphia Inquirer, St. Luke’s use of the technology “contributed to a 34% decline in cardiac arrests, and a 12% drop in patients crashing so hard and fast that they require rapid response transfers to the ICU between 2022 and 2024.” Cardiac arrest patients’ survival rate rose from 24% to 36% too, attributable to the speedy intervention that the device sets in motion.
“It’s helping the nurse feel supported,” Sonday said, “and it’s helping the patient’s safety.”
With results like these, medical professionals acknowledge that not only is technology and AI here to stay, but keeping up with its advancements is indeed crucial to providing Schuylkill County residents with the best and brightest of medical services.
“The future is really leveraging AI agents to assist us with patient access and patient education and understanding of their health,” Sonday said. “Leveraging technology to deliver information and care outside of the four walls of the hospital.”