One of the most climate-threatened corners of the planet, scientists fear Tuvalu will be uninhabitable within the next 80 years. — © AFP/File TORSTEN BLACKWOOD
Climate change causes more frequent and intense extreme weather events. One such area is with an increase rate of droughts. This affects everything from agriculture to microbial communities. A secondary factor is with how human societies respond to drought events in terms of land management.
Drought acts as a powerful driver of antimicrobial resistance (AMR) in soil, accelerating the evolution of superbugs. This is according to a 2026 Nature Microbiology study. The research reveals that dry conditions concentrate natural soil antibiotics, forcing bacteria to develop resistance to survive.
The scientists consistently observed metagenomic signatures of enrichment for antibiotic producers under drought conditions. Drought-tolerant communities tend to be dominated by specialised members of the Actinobacteriota, particularly the genus Streptomyces.
Temporal dynamics in microbial communities are primarily driven by seasonal and interannual variations in weather conditions. In this context:
In normal, moist soil, bacteria live in a relatively stable environment. But when soil dries out, water gets squeezed into tiny, isolated pockets. Bacteria get crowded together, nutrients become scarce and competition turns brutal. In these conditions, bacteria produce more antibiotics to attack each other, and more resistance genes emerge to help them survive.
Importantly, this environmental stressor directly correlates with higher rates of antibiotic-resistant infections in human hospitals. It also connects to climate change and adds another concern to the many others identified in relation to how human activity is adversely altering the planet.
Natural conditions vs climate altered situations
Microorganisms in soil naturally produce compounds that help them defend themselves against other competing microbes (among other functions). These natural compounds have been used by synthetic chemists as the scaffolds on which to build modern clinical antibiotics, and soil is a natural reservoir in which to discover new antibiotic candidates.
Yet as infectious pathogens can evolve resistance to clinical antibiotics, so too can bacterial species in soils can do the same, leading to ever-evolving competition.
The researchers found in every scenario they examined that antibiotic synthesis genes were more prevalent after a dry period and less prevalent after a drought ended (some of these can be transferred via the air). This occurred croplands, in grasslands, in forests, in wetlands; and in the U.S., in China, and in Switzerland – hence this is truly a global phenomenon.
 Mycobacterium tuberculosis (Public Health Image Library, NIAID, Image ID: 18139)
Mycobacterium tuberculosis (Public Health Image Library, NIAID, Image ID: 18139)
The primary factors with drought and resistance
The key factors, relating to drought and standard mechanisms for fuelling resistance, are:
- Natural Selection in Dry Soil: As soil dries, available moisture shrinks, causing natural antibiotics produced by soil microbes to become more concentrated. This intense, “lethal” environment eliminates sensitive bacteria, leaving only those with strong resistance genes.
- The Soil-Hospital Link: The study, which analysed soil from diverse regions alongside data from 116 countries, found that greater local aridity corresponds to higher rates of antibiotic-resistant infections in hospitals.
- Mechanisms of Resistance: The drought-induced stress not only increases the prevalence of genes for antibiotic resistance, but also those for antibiotic synthesis, indicating an active “evolutionary battlefield”.
- Impact on Soil Biodiversity: Drought disrupts microbial communities, dramatically reducing the growth of many bacterial groups (by ~50%), while favouring hardier, often resistant strains.
“No place is immune,” said Dianne Newman, the study’s senior author and a biologist at Caltech to Live Science. “If you have a pathogen arise in one part of the world, it very quickly spreads, so this is something of concern regardless of where you live.”
In terms of the actual mechanisms leading to bacteria becoming resistance, there is a mix of a newly identified factor together with established reasons as to why antimicrobial resistance occurs. Hence, the scientists pinpoint:
- Antibiotic Concentration: As soil moisture evaporates, the natural antibiotics produced by microbes to kill rivals remain behind, becoming more concentrated and lethal in the shrinking water film.
- Survival of the Fittest: This increased toxicity kills off sensitive bacteria while allowing those with resistance genes to survive and flourish.
- Genetic Enrichment: Studies across diverse ecosystems in China, Europe, and the USA consistently found that drier soils have higher abundances of genes for both producing and resisting antibiotics.
- Horizontal Gene Transfer: Bacteria can “swap” these resistance genes through horizontal gene transfer, allowing resistance developed in the soil to move into human pathogens.
Implications for Public Health
Many of the genes that confer antibiotic resistance in soil microbes were found, replicated exactly, in clinical pathogens known to escape antibiotics. These included the common hospital pathogens Enterococcus faecium, Klebsiella pneumoniae, Acinetobacter baumannii, Pseudomonas aeruginosa and species of Enterobacteria. This means what is occurring in one part of the world has a very real impact on an important area of human activity – the hospital.
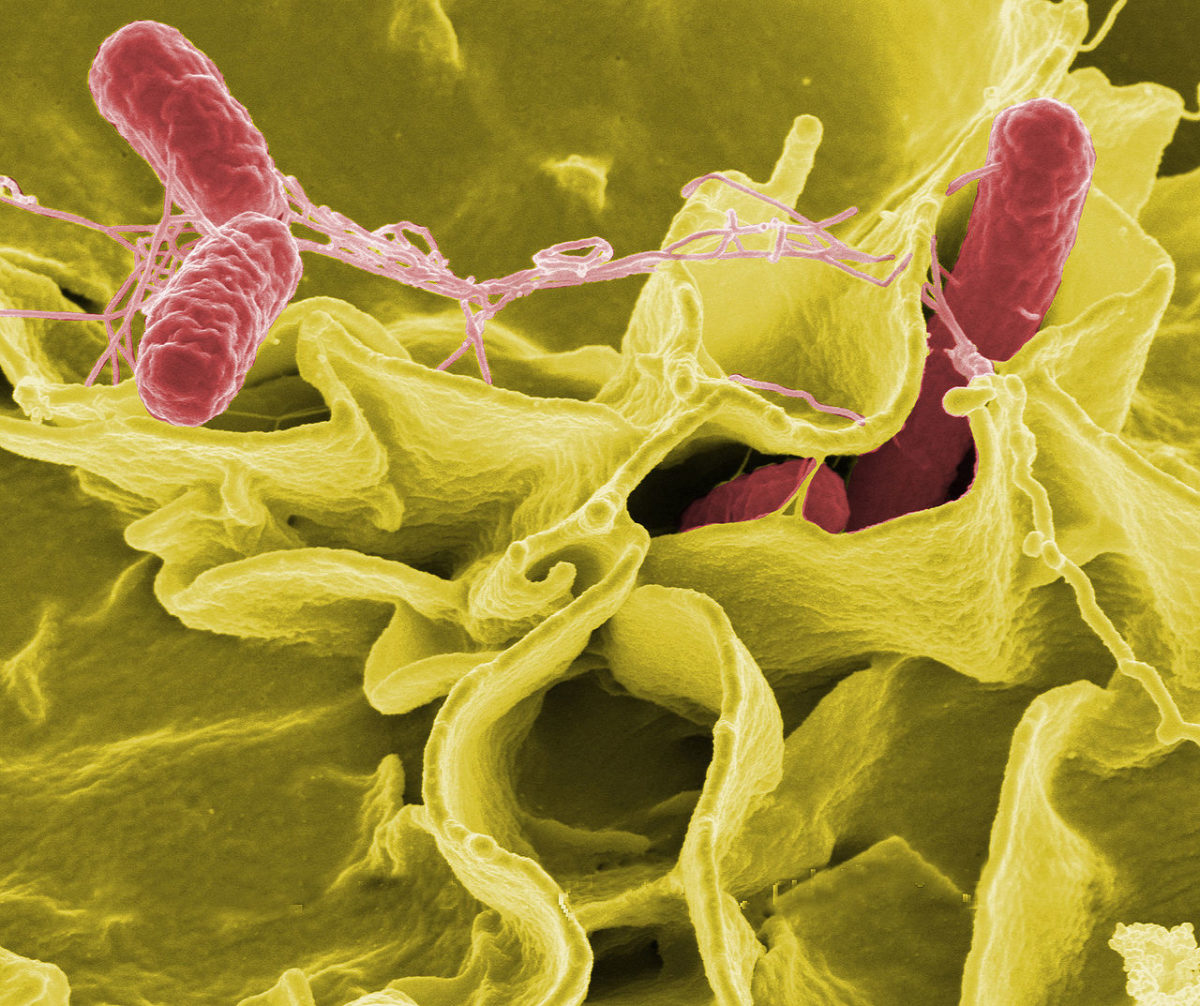 Bacteria electron micrograph (showing Salmonella typhimurium (red) invading cultured human cells). Image by NIAID / via Wikimedia / Public Domain
Bacteria electron micrograph (showing Salmonella typhimurium (red) invading cultured human cells). Image by NIAID / via Wikimedia / Public Domain
When comparing antibiotic resistance data from hospitals in 116 countries to local annual precipitation and mean temperature, the researchers found that greater aridity is associated with a higher average frequency of antibiotic resistance among clinical isolates.
Human, animal and environmental health are closely linked
The research highlights the general finding and an often overlooked link between environmental climate change and human health, forming a core component of “One Health” research. As droughts become more frequent and intense, the environmental reservoir of antibiotic resistance is expected to grow, potentially accelerating the global antimicrobial resistance crisis.
“One Health” research is a collaborative, multisectoral approach, driven by the World Health Organisation, that studies the interconnection between people, animals, plants, and their shared environment to improve health outcomes. It integrates expertise from human medicine, veterinary science, and ecology to prevent zoonotic diseases, combat antibiotic resistance, and manage environmental impacts on health.
The research group plans to use AI tools as he next phase to discover and understand the mechanisms that bacteria utilize to resist and modify antibiotics.
The research paper is titled “Drought drives elevated antibiotic resistance across soils” and in appears in the journal Nature.

