The pathophysiology of corneal frostbite differs significantly from typical extremity frostbite. While classical frostbite primarily involves cold-induced vascular damage leading to ischemic perfusion injury [1], the unique anatomical and physiological characteristics of the cornea result in a distinct pathological process.
The cornea’s avascular nature [5] necessitates alternative mechanisms for thermal regulation and nutrient supply. These are provided by both the peripheral vessels at the corneal margin and the anterior aqueous humor [2, 5]. The absence of precapillary sphincters in the choroid ensures consistent blood flow [2], maintaining intraocular compartment temperatures near core body temperature. Even in extreme polar conditions, the anterior chamber maintains a stable temperature of approximately 37 °C [2]. Furthermore, decreasing ambient temperatures enhance aqueous circulation near the cornea [2], creating thermal currents that help resist temperature reduction. Experimental evidence has shown that corneal surface temperature can maintain 24.3 °C even when exposed to −40 °C air temperature for 30 min, well above the tissue freezing point of −0.53 °C to −0.65 °C [2].
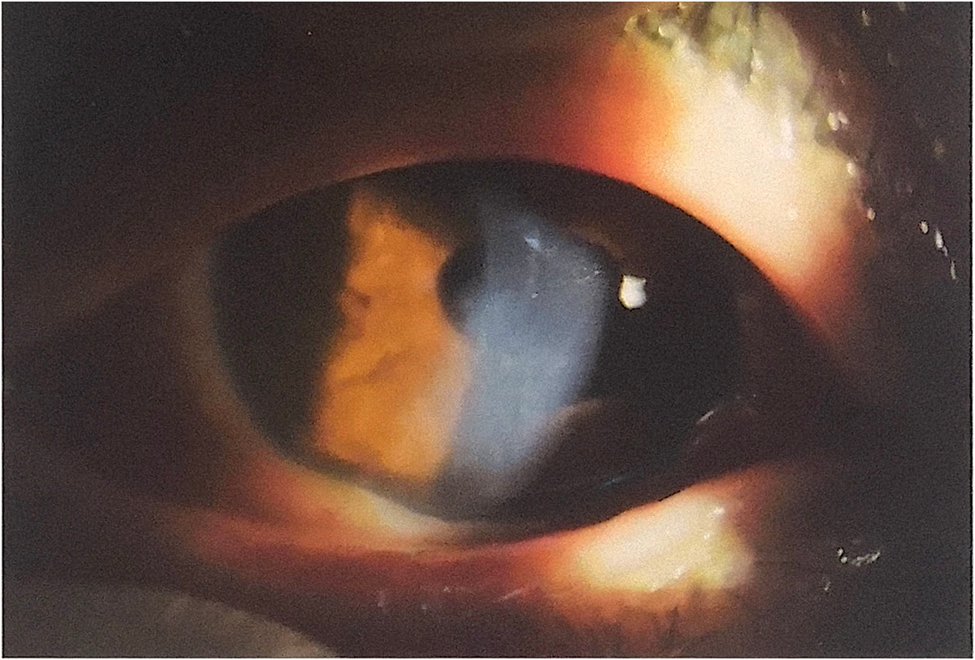
Despite these protective mechanisms, prolonged exposure to extreme conditions can overcome these natural defenses. In this case, the three-hour exposure to temperatures between − 16 °C and − 23 °C, combined with significant wind speed, proved sufficient to cause corneal injury. While ischemia may not be the primary mechanism of injury, the formation of ice crystals can directly damage both the epithelial and endothelial layers, explaining the observed corneal staining and edema.
The persistent endothelial scar and prolonged corneal edema observed in this case can be attributed to several factors. First, low temperatures suppress sodium-potassium pump activity [6], compromising the endothelium’s dehydration function and resulting in corneal edema. Second, corneal endothelial cells lack mitotic activity in vivo, requiring surviving cells to spread and compensate for damaged areas [6], potentially explaining the persistent scar formation. Finally, the endothelium demonstrates sensitivity to cold injury, with research showing that even brief exposure to −80 °C for 3 s can induce corneal endothelial decompensation and stable bullous keratopathy in experimental models [7].
Previous similar cases have been reported, including a marathon runner who developed eye injury under conditions of high wind speeds and near-zero temperatures [8]. This runner similarly wore no eye protection during prolonged running, had no significant medical history, and developed similar symptoms immediately after running. The reporting doctors also suggested that wind speed might have exacerbated the cold damage to the cornea. Unfortunately, since the reporting physicians were not ophthalmologists, the ocular assessment of this patient was relatively simple, providing only one external photograph with no detailed treatment records. However, we can still observe obvious corneal edema in the central-inferior region of the runner’s left eye in the photograph. This type of corneal damage occurring immediately after prolonged exposure to low-temperature, high-wind environments should be distinguished from diffuse corneal epithelial punctate staining that appears several hours after snow environment exposure [9]. From our perspective, the latter condition is more Likely snow blindness, which is corneal epithelial damage caused by ultraviolet Light reflected from snow. Snow blindness typically does not involve the corneal stroma and endothelium, with good prognosis and rapid recovery within 48 h. We believe that low temperature is likely not the primary causative factor in the latter type of patients.
Besides, the treatment administered in this case offers valuable insights. The initial management by local ophthalmologists included topical 50% glucose and Vitamin C. Hyperosmolar eye drops are known to reduce corneal edema [10], and topical Vitamin C has been reported to aid corneal wound healing [11]. These may explain the treatment choice. However, corneal edema persisted in the right eye and seemingly responded better to topical steroids at our institution. We speculate that steroid therapy may be more effective in patients with corneal frostbite and significant edema.
This case report has limitations. Without pre-frostbite ocular images, we cannot completely exclude a pre-existing endothelial scar. While this case report was limited by the unavailability of corneal confocal microscopy and some imaging resolution constraints due to geographical factors, it provides a rare documentation of environmental cold-induced corneal injury. The findings contribute valuable insights to the clinical management and research understanding of corneal frostbite.