With the looming end of pandemic-era credits, families on Covered California health plans are seeing their premiums go up drastically.
Some say they’re considering dropping health insurance — a move that local officials say could end up increasing health care costs for everyone.
This month many of the 82,000 Alameda County residents who get health insurance through Covered California are experiencing sticker shock when they see how high their premiums will be in 2026.
“I have a knot in my stomach every single day,” said Rachel Rosekind, 49, an El Cerrito mother whose monthly premium will go from $0 to $2,500 a month for her family of four.
Rosekind, a self-employed freelancer, said she was fortunate during the pandemic to qualify for a $0 premium for a Kaiser high-deductible plan through the state’s health insurance exchange. Open enrollment began Nov. 1 and ends Jan. 31, 2026.
However, when she went to re-enroll this year, she discovered that they’re now facing a daunting monthly payment.
“We could not afford $30,000 a year in insurance without going into medical debt,” Rosekind said.
 Self-employed freelancer Rachel Rosekind of El Cerrito is scrambling to figure out how her family can afford to pay $2,500 a month for health insurance. Courtesy of Rachel Rosekind
Self-employed freelancer Rachel Rosekind of El Cerrito is scrambling to figure out how her family can afford to pay $2,500 a month for health insurance. Courtesy of Rachel Rosekind
She and her family are rushing to finish all of their preventative care under their existing plan by the end of the year. She got a mammogram last month and booked well visits for her children in December.
Rosekind is the sole income-earner for her family. She and her husband have two daughters, who are 13 and 10.
The rising premiums have “ motivated me to get everything that I can done by the end of the year because it is such a big question mark around what we’re going to do,” Rosekind said.
Why are health premiums going up in 2026?
The Covered California health exchange is a marketplace where Californians can shop for health insurance. It was created to offer subsidized Obamacare health insurance plans.
“We are unique among marketplaces,” said Jessica Altman, executive director of Covered California. Covered California spends “a lot of our time negotiating with our health plans setting higher bars for our health plans across different areas of work, trying to improve quality, equity, access.”
 Jessica Altman, executive director of Covered California, spoke to the media at a press conference last month to discuss the enrollment process and health insurance issues the state will face in 2026. Courtesy of Covered California
Jessica Altman, executive director of Covered California, spoke to the media at a press conference last month to discuss the enrollment process and health insurance issues the state will face in 2026. Courtesy of Covered California
Of the 82,150 Alameda County residents who buy insurance through Covered California, 74,690 people qualified for lower premiums due to pandemic-era subsidies, known as Enhanced Premium Tax Credits, as of June.
The question of whether or not these credits will be continued was at the heart of the federal government shutdown and while the shutdown is over, the issue hasn’t been resolved. It remains unclear if the Republicans and the Trump Administration will extend those credits.
For context, the American Rescue Plan Act authorized, and the Inflation Reduction Act extended tax credits for Obamacare health insurance plans during the pandemic during, providing California with $2.5 billion in subsidies, Altman said.
During the pandemic, the federal government also eliminated income-based restrictions for financial assistance. Previously, people making more than 400% of the federal poverty level, or $65,000 a year, did not qualify for a subsidized plan. But pandemic-era regulations removed that income cap. No one was expected to pay more than 8.5% of their income toward healthcare premiums, she said.
“Nationally, enrollment in marketplaces more than doubled since doing so,” Altman said. In California, “this has not just improved affordability, but it [has] gotten more people covered and we’re at a record-low uninsured rate.”
However, both the tax credits and income qualifications are set to expire at the end of this year.
“Without an extension of the Enhanced Premium Tax Credits, monthly premiums are projected to rise by 97% on average for more than 1.7 million Californians enrolled and receiving financial assistance through Covered California,” according to a Covered California press release issued Nov. 13.
Families are scrambling to figure out if they can afford higher premiums
Every year, Guillermo Jimenez helps more than 100 East Bay families apply for health insurance through the Covered California Health Exchange.
This open enrollment season, the insurance broker has seen sharp increases in his clients’ monthly premiums. For 2026, monthly premiums have increased by as much as 150% from 2025 rates.
Not all his clients can afford to pay this. Two clients have already dropped their health insurance altogether.
 East Bay insurance broker Guillermo Jimenez says he expects a number of his clients will drop their health insurance in 2026 due to rising premiums. His own health premiums are more than doubling for his family of four. Courtesy: Richmond Main Street Initiative
East Bay insurance broker Guillermo Jimenez says he expects a number of his clients will drop their health insurance in 2026 due to rising premiums. His own health premiums are more than doubling for his family of four. Courtesy: Richmond Main Street Initiative
“They will go [through] 2026 without coverage, even when they know they have to pay a penalty on the taxes,” Jimenez said, referring to an annual state penalty that’s assessed against residents who don’t have health insurance.
Jimenez expects that more of his clients will drop health insurance.
Rosekind is facing that exact decision. She doesn’t want to give up health insurance, but she is unsure what to cut out of her budget to make room for insurance premiums.
“We’re currently in a little bit of a fight (or) flight mode,” she said, “because we don’t really know what we’re going to do.”
For example, to afford the new health insurance premiums, Rosekind is considering cutting back on the healthy food she buys.
“We eat organic food and healthy food, which is one of the reasons we stay really healthy and don’t use as many health services,” she said. “But that might be a choice I would have to revisit to start to understand what the impacts are of rising health costs.”
She is even thinking of moving away from the Bay Area to a place with a lower cost of living. But it would be difficult to continue her work if she moves.
“I do a lot of really county-specific work that requires a lot of local knowledge and local connections that I’ve built up over the course of many years,” Rosekind said.
Altman acknowledged this is facing many on an individual level.
“It is a tragic, sort of rolling of the dice and hoping that you will not need healthcare, that you will be healthy,” Altman said. But the systemic repercussions of this are even greater.
Having more uninsured people burdens the whole healthcare system
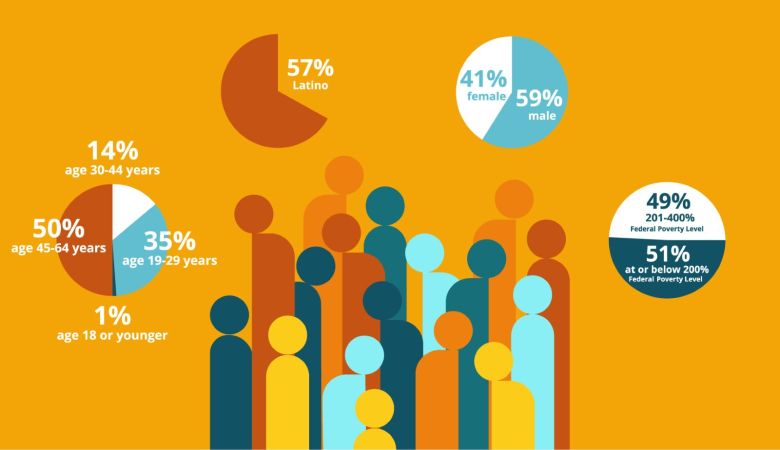 This graphic showing the demographic breakdown of uninsured Californians points out that the majority of them are Latino. Courtesy: Covered California
This graphic showing the demographic breakdown of uninsured Californians points out that the majority of them are Latino. Courtesy: Covered California
In addition to helping others buy health insurance from Covered California, Jimenez buys his health insurance through the marketplace. He said he can get health insurance through his employer, but it was less expensive for him to buy coverage for his family of four through the health exchange.
Jimenez’s Covered California premium will increase 124% — from $205 to $461 monthly. Like Rosekind, he currently has a Kaiser plan, liking it’s easy access (it has a Richmond campus) and low cost. He estimates that 95% of his clients also choose Kaiser plans for the same reason.
Kaiser is also concerned about the expiring tax credits.
It is a tragic, sort of rolling of the dice and hoping that you will not need healthcare, that you will be healthy.” — Jessica Altman, executive director of Covered California, on the repercussions of more people going uninsured
“The scheduled expiration of the enhanced premium tax credits could increase out-of-pocket costs for enrollees. As a result, many may face higher costs, and some may struggle to keep their coverage,” said Kaiser Permanente in a written statement.
“Some individuals who are healthier and have lower health needs will likely drop coverage, leaving higher-risk individuals in the market and contributing to future rate increases,” the statement continued.
Altman said that one of the implications of a larger uninsured population is reduction of services and closing of rural clinics.
“ When you get to that point-of-access issues, the hospital serves everyone, not just covered California enrollees. And so those impacts are felt across the community,” she said.
This holiday season, Rosekind, Jimenez, and many others will be tightening their belts.
“ I won’t buy anything for the family,” Jimenez said about Christmas gifts. He hopes to make it up to them another way.
Congress not extending the tax credits “ forces me into an impossible position for me and my family,” said Rosekind, “as I’m sure it does for countless families across the country who are facing the same issues right now.”
“*” indicates required fields

