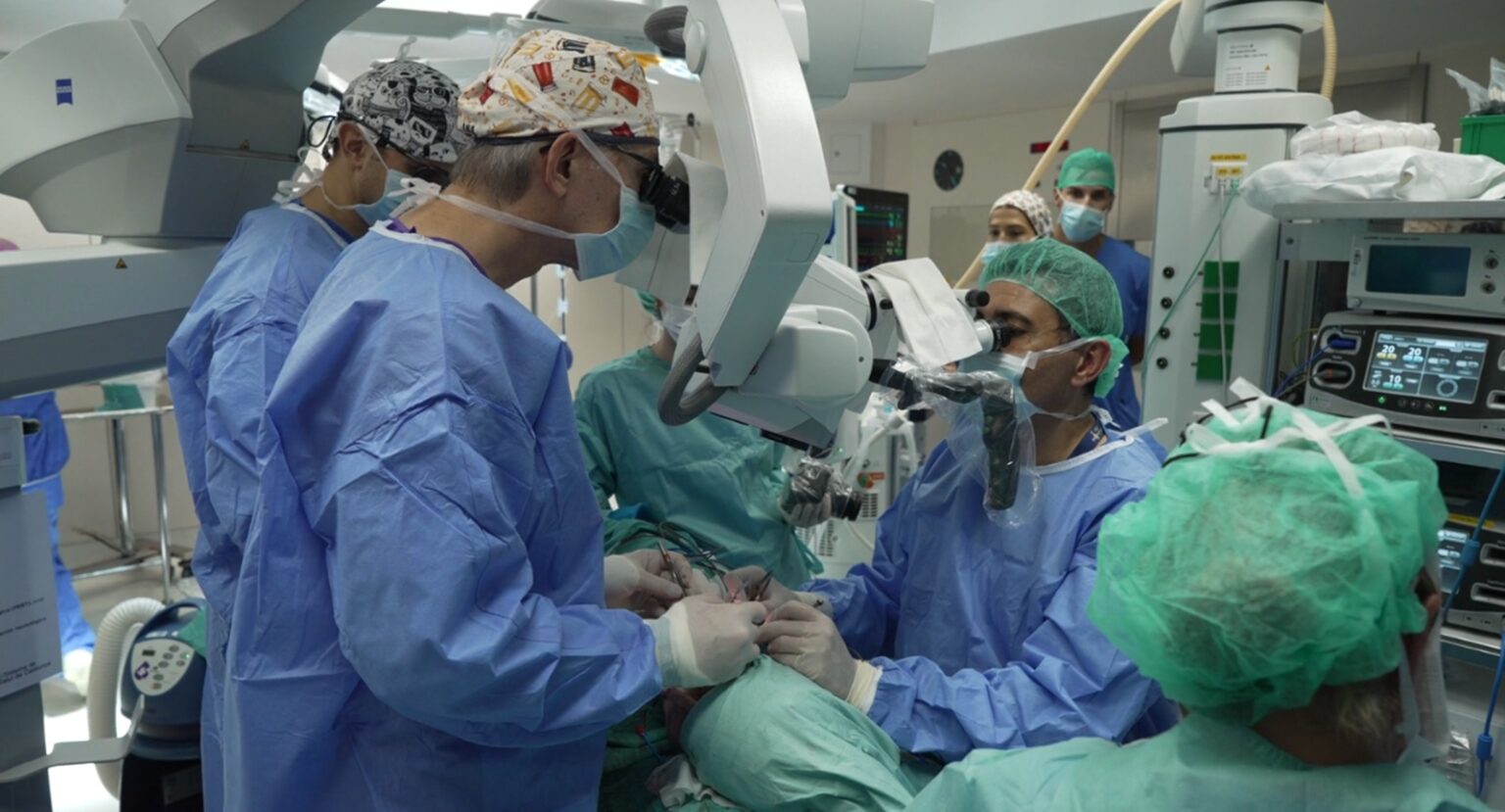
Spain performs first face transplant from a euthanasia donor. The case links euthanasia and organ donation, sparking debate in Colombia. Dr. Joan Pere Barret (center) leads the surgical team during the world’s first face transplant using a donor who underwent euthanasia. Credit: Vall d’Hebron University Hospital (for editorial purposes only).
Spain has performed the world’s first face transplant using an organ donor who previously accessed euthanasia, a medical milestone that immediately intersects with Colombia’s own end-of-life and transplant debates. The surgery took place at Vall d’Hebron University Hospital in Barcelona, one of the few centers with experience in this type of highly complex procedure.
The recipient is a woman who lost much of the central part of her face after a severe bacterial infection destroyed soft tissues and bone and left her unable to eat, speak or socialize normally. Surgeons classified the procedure as a type I face transplant, focused on the nose, lips, maxilla and surrounding tissue, a category that targets function and basic appearance rather than a full facial replacement.
Vall d’Hebron mobilized around 100 professionals from surgery, transplantation, anesthesiology, immunology, intensive care, psychiatry, psychology, rehabilitation and pathology for the case. The hospital stressed that this kind of operation remains exceptional, with only 54 face transplants documented worldwide and about 20 centers capable of offering them.
A donor who chose euthanasia and donation
The donor had requested euthanasia after meeting the legal criteria in Spain and, at the same time, had authorized donation of organs and tissues, including the face. Hospital officials described that decision as an act of generosity and psychological maturity, because the same person who decided to end a difficult life also decided to make another person’s life more bearable.
Engineers and surgeons used CT scans of the donor and recipient to design the operation, building 3D models of both skulls and printing guides for bone cuts and placement. They also created a semi-rigid silicone mask to reconstruct the donor’s face for the funeral, a detail that addresses a sensitive aspect of donation: the family’s right to say goodbye without visible mutilation.
The transplant itself required between 15 and 24 hours in the operating room, depending on how the stages are counted, including bone work, vascular connections, nerve repair and soft tissue closure. As a reminder, face transplants do not simply “attach” a new face; they attempt to connect blood supply and nerves so that the recipient can eventually move, feel and express again.
Colombia faces the same ethical crossroads
The recipient spent one month in hospital, first in intensive care and then in the burns and rehabilitation unit, a shorter time than the three months needed for Vall d’Hebron’s first face transplant in 2010 and two months in 2015. She now follows a rehabilitation program to regain facial movement, a process that can take months or years but has improved with surgical experience.
Colombia has no direct parallel to face transplantation, but the country has active transplant infrastructure and has performed 1,358 transplants in 2024, according to the National Institute of Health. Colombians will recognize the ethical tension in this case because euthanasia has been legal since 1997, and the Constitutional Court has progressively expanded access through rulings such as C-239 of 1997 and T-970 of 2021.
However, Colombia’s system separates the decision to die from the decision to donate. Article 14 of Law 73 of 1988 regulates organ donation after death, and euthanasia patients must follow a protocol that includes prior consent for donation, but no case has yet combined both in a high-profile way like Spain’s.
To this day, Colombian doctors and ethicists debate whether euthanasia donors should be treated differently from other deceased donors, especially when the face or other visible tissues are involved. The Ministry of Health has not issued specific guidelines on face or tissue donation from euthanasia cases, leaving hospitals to follow general consent rules.
What Spain’s case means for Colombia
Worth noting is that Spain’s surgery used advanced 3D modeling and printed guides, technologies that Colombian hospitals such as Fundación Cardioinfantil in Bogotá already apply in complex transplants. However, Colombia’s transplant system faces capacity limits, with over 4,000 patients waiting for organs each year and a 50% rejection rate due to family refusal or logistics.
In reality, the Barcelona case will likely reach Colombian courts and Congress soon, because it touches on two expanding frontiers: euthanasia access and organ allocation. The Constitutional Court could use it as a reference when reviewing cases about donor consent from patients with terminal illness or mental suffering, the same categories covered in recent rulings.
This will be a test of whether Colombia’s legal framework can handle the intersection of euthanasia and donation without creating new barriers or conflicts. If more cases follow Europe’s lead, Colombian hospitals may need updated protocols to manage donor families, psychological support, and the public debate that comes with visible transplants.