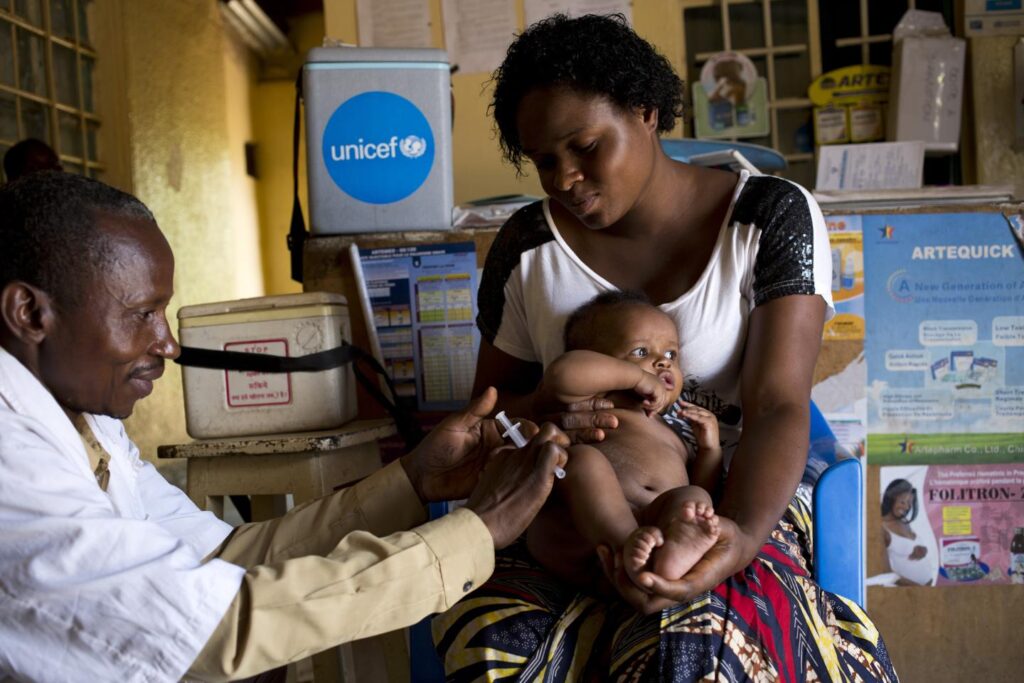
In the quiet town of Săcele, Transylvania, the corridor of Dr. Mirela Csabai’s clinic serves as a grim barometer for a continent-wide health emergency. By mid-morning, parents pack the narrow walkway, clutching children who, in better times, would be protected by the simple, long-established barrier of a vaccine. Today, however, that shield is crumbling.
This scene, repeated in health centers across Romania, marks the epicenter of a burgeoning health crisis that threatens to undo decades of progress. Between 2023 and 2025, Romania recorded more than 35,000 cases of measles and at least 30 deaths, most of them infants. This surge, which accounted for 87% of all measles cases in the European Union in 2024, is not merely a regional outlier it is a warning flare for global health security, highlighting how quickly even modern medical infrastructure can be undermined by apathy, misinformation, and systemic neglect.
The Anatomy of a Public Health Collapse
The resurgence of measles in Romania is a multi-layered tragedy, driven by a convergence of shifting social attitudes and infrastructural decay. While historically the country maintained high immunization rates—once reaching a record 98% in 1999—that consensus has fractured. Experts at the National Institute of Public Health point to a marked decline in uptake since the Covid-19 pandemic, as vaccine fatigue evolved into entrenched hesitancy.
The mechanics of this decline are starkly visible in the immunization data. To achieve herd immunity, the World Health Organization (WHO) mandates a 95% vaccination threshold. Romania is operating far below this safety margin, with consequences that extend well beyond its borders.
- First Dose Coverage (14–18 months): Currently 81% nationally, down from historical highs.
- Second Dose Coverage (at age 5): Barely exceeding 60%, with some rural communities reporting levels as low as 20%.
- Epidemic Toll (2023–2025): 35,736 confirmed cases 27,720 infections in children under 15 30 confirmed fatalities.
- Regional Concentration: Argeș county records the lowest vaccination coverage at 23.7%.
Dr. Mihai Negrea, an epidemiologist, emphasizes that this is not just about the anti-vaccination movement it is about the “lost” vaccination, where logistical bottlenecks—such as the cessation of school-based immunization programs and an over-reliance on a shrinking pool of general practitioners—mean parents often fail to return for the critical second dose.
The Global-Local Bridge: Lessons for Nairobi
While the drivers of the crisis in Romania—misinformation and social apathy—may seem distinct from the challenges faced in East Africa, the underlying vulnerability is shared. In Kenya, the conversation around immunization has focused heavily on access and infrastructure. Despite strong progress, where coverage for basic antigens reached 80% among infants aged 12 to 23 months, pockets of susceptibility remain, particularly in urban informal settlements like Mathare, where routine immunization reports have occasionally shown coverage rates hovering around 50% for measles.
The Rwandan and Romanian experiences offer a mirror for Kenya. While Romania struggles with a populace turning away from science, Kenyan health authorities are aggressively fighting to keep children from falling behind due to “missed opportunities”—the failure of health facilities to administer all necessary doses during a single visit. The National Vaccination and Immunization Programme (NVIP) in Kenya has recognized that relying on 10-dose vials led to wastage and stockouts, prompting a shift to 5-dose vials to boost uptake and minimize the distance between the vial and the arm. Whether the threat is a lack of clinics in a remote Kenyan county or a lack of trust in a Transylvanian town, the result is the same: the virus finds the unvaccinated.
The Cost of Inaction
Measles remains one of the most contagious diseases known to science. A single infected individual can transmit the virus to as many as 18 others lacking immunity. As the virus travels through under-vaccinated populations, it does more than cause fever and rashes it “erases” the immune system’s memory of how to fight other infections, leaving survivors vulnerable for months or years to follow.
The crisis has drawn a hard line for European policymakers. In January 2026, the WHO reported that several European nations had lost their measles-free status, a devastating blow to a region that once led the world in disease eradication. This loss of status serves as a “canary in the coal mine” for the world. If developed nations cannot protect their most vulnerable from a preventable disease, the global ambition to eliminate measles by 2030 is at profound risk.
For the parents sitting in Dr. Csabai’s corridor, the abstract data points translate into sleepless nights and hospital wards. Every percentage point drop in national coverage represents thousands of children left defenseless. Until health systems can bridge the gap between policy and the reality on the ground—by replacing misinformation with trust and bureaucracy with accessibility—the powder keg will remain lit.
The resurgence of this once-conquered disease is a sobering reminder that immunization is not a static achievement but a continuous, hard-won responsibility. As the world watches Romania, the question for other nations, including Kenya, is whether they will wait for a similar crisis to act, or if they will fortify their immunization defenses while the calm still holds.