Mental health professionals (MHPs) play a crucial role in supporting individuals with psychological challenges. However, they themselves are not immune to the emotional demands and stress of their work. Studies indicate that the mental health field is associated with high levels of stress, which can lead to adverse psychological outcomes such as depression, anxiety, and burnout [1]. Understanding the complex interplay of these factors is essential to creating effective strategies that support the well-being of MHPs and, by extension, the individuals they serve.
Burnout, a term introduced by Freudenberger and North, describes a state of emotional exhaustion, depersonalization, and reduced personal efficacy arising from chronic workplace stress [1]. Among mental health professionals, burnout is an increasingly recognized concern due to the emotionally intense nature of their work. Prolonged job stress can lead to mental and physical exhaustion, depersonalization, and dissatisfaction with one’s achievements, all key facets of burnout [2]. MHPs are particularly vulnerable to burnout, depression, and anxiety due to their high-stress environments and exposure to the suffering of others [3, 4].
Stress, in this context, occurs when tension persists because an individual cannot apply effective coping techniques. Although stress, anxiety, and depression are conceptually distinct, they share overlapping symptoms that may contribute to the progression from one condition to another [4]. Mental health professionals face unique stressors, such as vicarious trauma from empathetic involvement with distressed patients, high workloads, managing aggressive or suicidal patients, and often limited access to adequate support. These factors contribute to the high rates of mental health challenges within this field [8, 9].
Medical professionals, and especially MHPs, are thus at elevated risk of burnout, despite often possessing better-than-average physical health [5,6,7]. Recent studies highlight that psychiatrists, for example, report higher levels of emotional exhaustion, severe depression, and stress compared to other medical specialists, such as family doctors and surgeons [9]. The Medscape poll underscores the gravity of the issue, revealing that 42% of mental health workers experience burnout, with female psychiatrists at even higher risk [11, 12].
The consequences of burnout are far-reaching. Poorly managed burnout has been linked to low organizational commitment, absenteeism, high turnover, and interpersonal conflicts. It affects not only the well-being of the professionals but also impacts the quality of patient care, team dynamics, and even family life. Furthermore, burnout is associated with serious physical health risks, including coronary heart disease, musculoskeletal discomfort, type 2 diabetes, and suicidal ideation [13,14,15,16]
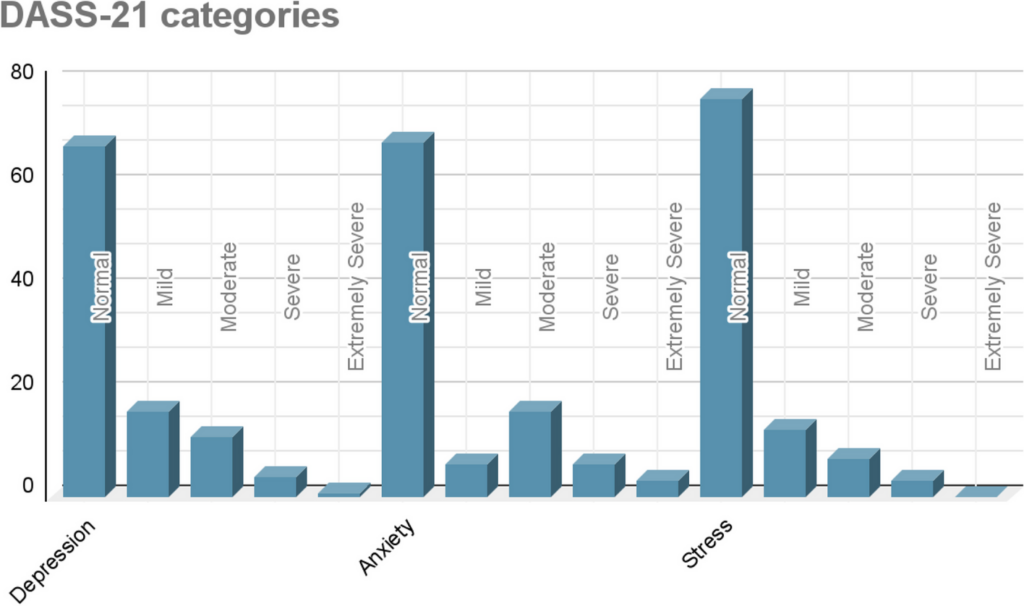
Given these significant challenges, this study aims to explore the prevalence and interrelationships of depression, anxiety, stress, and burnout among mental health professionals in Khartoum, Sudan. By shedding light on the mental health landscape of MHPs, the study can contribute to the development of effective support strategies, ultimately benefiting both these professionals and the broader communities they serve.